Reexamining Cancer Screening to Enhance Longevity
The Importance of Early Detection
As medical science progresses towards the goal of enhancing human longevity, addressing mortality from cancer has emerged as a key priority. Unlike some other prevalent diseases that reduce lifespan, cancer may more uniquely impact lifespan while leaving healthspan intact in early stages. As such, host Dr. Peter Attia argues that minimizing cancer deaths is a “pillar” of longevity-focused medicine.
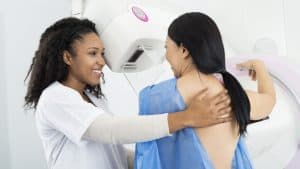
Within this context, early detection through screening allows for more successful cancer treatment compared to detecting advanced stage disease. Attia cites statistics showing 5-year breast cancer survival rates of 99% for localized tumors versus only 25% once cancer has metastasized. The significantly higher odds of survival spotlight why screening techniques to catch cancer sooner may be so valuable.
Interpreting Screening Approaches
However, Attia notes screening does carry downsides of financial expense and the risk of false positive or false negative test results. To help weigh screening benefits versus potential harms, guest expert Dr. Bob Kaplan highlights the utility of metrics like sensitivity, specificity, positive predictive value, and negative predictive value.
Sensitivity refers to how accurately a screening test correctly identifies people who have a medical condition. Specificity measures how well a test correctly reports negative results for healthy individuals without the condition. The positive predictive value captures what proportion of positive test results reflect the underlying presence of disease, while the negative predictive value conveys the likelihood someone testing negative is actually disease-free.
Kaplan explains these parameters help characterize any screening method’s real-world performance. Reviewing cancer screens through this lens empowers patients and providers to make informed decisions aligned with personal health priorities.
Opportunities to Refine Approaches
Attia and Kaplan explore how combining multiple screening modalities may improve predictive accuracy. For instance, while assessing blood-based biomarkers, imaging tests, and genetic risk profiling individually have pros and cons, layering these approaches could allow their respective strengths to complement each other.
This underscores the idea that screening techniques continue to evolve. Especially for complex conditions like cancer spanning hundreds of subtypes, the podcast guests express optimism about enhancing early detection through purposefully categorizing cancers and selecting tailored screening protocols.
By reexamining core assumptions around prevailing screening norms, while also broadening understanding of emerging innovations, patients and providers can collaboratively determine suited options for monitoring cancer risk on an individualized basis.
Takeaways for Patients and Providers
- Early cancer detection demonstrably improves treatment efficacy and survival odds, supporting screening to enable finding tumors sooner.
- Metrics like sensitivity and specificity help characterize real-world performance of any screening method to guide appropriate interpretation.
- Layering multiple screening approaches may leverage their respective strengths to increase predictive accuracy.
- Categorizing cancers combined with personalized screening allows optimizing early detection.
- Reevaluating established protocols alongside new innovations opens possibilities to refine screening.
By reconsidering screening fundamentals while also tracking cutting-edge progress, stakeholders across healthcare can unravel the full promise of early detection to combat cancer. Patients can crucially play an active role through education, shared decision-making, and tailored action to protect health.
\n\n